Arthrosamid Injection Side Effects: What Are the Risks and How Common Are They?

Knee osteoarthritis affects millions of adults across the United Kingdom. According to Versus Arthritis, over 8.75 million people in the UK have sought treatment for osteoarthritis. Many of them reach a point where standard options — physiotherapy, anti-inflammatory medication, and steroid injections — stop providing adequate relief. For these patients, Arthrosamid has emerged as a newer injectable treatment that promises longer-lasting results. But before any patient commits to this procedure, they deserve a clear and honest account of the risks involved.
This article covers what Arthrosamid is, what the known side effects are, how common those side effects occur, and what patients in the UK need to understand before proceeding.
What Is Arthrosamid?
Arthrosamid is a polyacrylamide hydrogel. It consists of 2.5% cross-linked polyacrylamide and 97.5% water. A clinician injects it directly into the knee joint using ultrasound guidance. The hydrogel integrates with the synovial membrane — the tissue lining the inside of the joint — and works as a cushioning agent.
Unlike steroid injections, which offer temporary anti-inflammatory relief, Arthrosamid is not biodegradable.The body does not dissolve or absorb it over time. The goal is to provide sustained pain relief and improve function in patients with mild to moderate knee osteoarthritis.
It is a single injection.They designed it to last. That permanence is central to both its appeal and to the questions patients rightly ask about its safety.
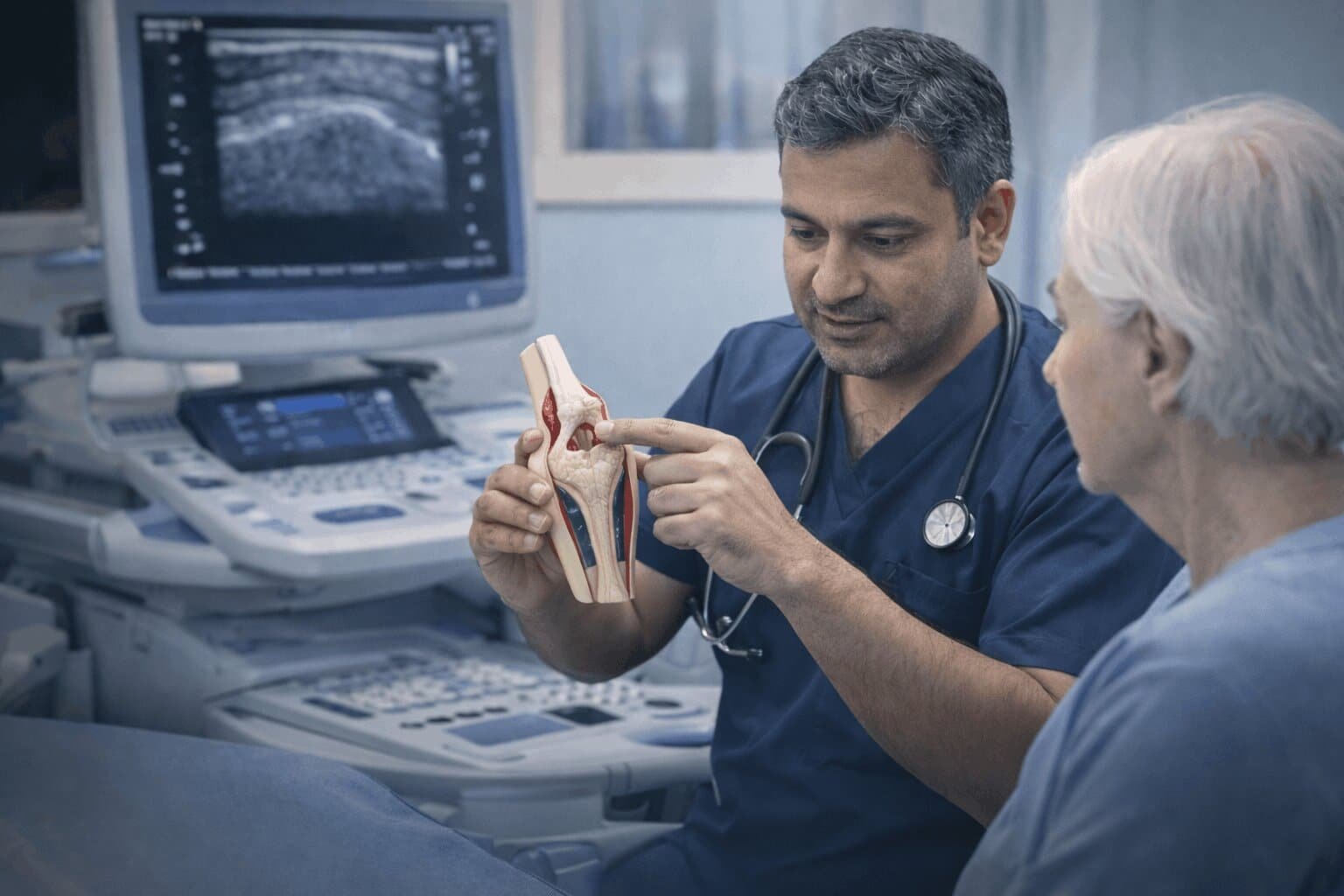
Is Arthrosamid Approved in the UK?
Arthrosamid holds a CE Mark, meaning it meets the standards required for medical devices sold within Europe. It is available as a licensed medical device in the United Kingdom.
It is important to understand that Arthrosamid is classified as a medical device, not a pharmaceutical drug. This matters because its regulatory pathway differs from medicines that go through the MHRA’s drug licensing process.
The NHS does not currently fund Arthrosamid. NICE — the National Institute for Health and Care Excellence, which advises the NHS on clinical and cost effectiveness — has not issued a technology appraisal recommending it for routine commissioning. This means every patient who receives an Arthrosamid injection in the UK does so through a private clinic, at their own expense.
That absence of NHS funding does not mean the treatment is unsafe or ineffective. It reflects the stage of the evidence base. Long-term post-market data is still accumulating, and NICE requires robust, independently reproduced evidence before recommending wide adoption.
What Does the Clinical Evidence Say?
The most significant clinical trial for Arthrosamid is the TACIT trial, a randomized controlled study conducted in Denmark. It compared Arthrosamid to a saline placebo injection in patients with knee osteoarthritis. The trial showed statistically significant improvements in pain and function scores at 26 weeks. Follow-up data at one and two years suggested that a meaningful proportion of patients-maintained benefit over time.
A peer-reviewed observational study also reported sustained improvements lasting up to two years following a single injection in some patients.
These are credible results. However, the published evidence base remains relatively small.The sample sizes in existing studies are modest compared with treatments that carry decades of post-market data, researchers found.This is not unusual for newer treatments, but it is an honest limitation that patients should factor into their decision.
Arthrosamid Injection Side Effects: The Full Picture
This is what most patients want to know most. The side effect profile of Arthrosamid, based on published clinical trial data and manufacturer reporting, divides into three broad categories: common and mild, less common, and rare but serious.
Common Side Effects After Arthrosamid Injection
Temporary increase in knee pain is the most frequently reported side effect. Many patients experience a worsening of pain in the days immediately following the injection. Clinicians call this a post-injection flare. It typically resolves within one to two weeks and does not indicate treatment failure.
Swelling of the knee joint is also commonly reported. Any intra-articular injection introduces a foreign substance into the joint space, and the body produces an initial inflammatory response. This swelling is generally mild to moderate and settles without specific treatment.
Stiffness — reduced ease of movement in the knee — affects some patients in the first week or two. This improves as the early inflammatory response settles.
These three reactions are expected and predictable. They are part of the body’s normal response to the procedure. They are not signs that something has gone wrong.
Less Common Side Effects
Joint effusion — an accumulation of fluid within the knee joint — occurs in some patients. In most cases it resolves on its own. Occasionally, a clinician needs to drain the fluid through a procedure called aspiration.
Localised warmth and redness around the knee is documented in some cases. It reflects local inflammation and generally resolves within a few days to a week.
Bruising at the injection site is possible with any needle-based procedure and is usually minor.
Rare but Serious Risks
Septic arthritis — infection within the joint — is the most serious potential complication of any intra-articular injection. It is rare, but it is a medical emergency when it occurs. The joint becomes rapidly painful, swollen, warm, and the patient may develop a fever. Patients must seek urgent medical attention if these signs appear, particularly if they develop several days after the initial post-injection period has settled.
Trained clinicians significantly minimize the risk of infection when they perform the procedure in a properly equipped, sterile clinical environment.
Researchers have not reported allergic or hypersensitivity reactions to polyacrylamide as a common finding in Arthrosamid clinical trials, although such reactions are theoretically possible. Patients with known sensitivities to the components of the hydrogel should raise this with their clinician before proceeding.
Hydrogel migration is a theoretical concern associated with polyacrylamide gels used in other medical contexts. In the context of intra-articular knee injections specifically, published Arthrosamid trial data does not identify this as a clinically significant problem. However, because the material is permanent, patients should understand that any complication that does arise cannot be simply reversed by the substance being absorbed over time.
How Common Are These Side Effects?
In the TACIT trial and related observational studies, the vast majority of reported adverse events were mild and resolved without intervention. The rates of serious adverse events were low and broadly consistent with those seen with other intra-articular injection procedures.
To put this in context: corticosteroid injections — widely used for decades and available on the NHS — carry their own risk of infection, cartilage damage with repeated use, and post-injection flare. Hyaluronic acid injections similarly produce local reactions in a proportion of patients. Arthrosamid’s side effect profile does not appear substantially worse than these established treatments, though longer-term surveillance data would provide greater certainty.
The permanent nature of Arthrosamid is the key differentiator. If a steroid injection causes a reaction, the steroid is metabolized and cleared within weeks. Arthrosamid remains. This is why accurate patient selection and careful technique matter as much as the product itself.
Who Is Not Suitable for Arthrosamid?
Not every patient with knee osteoarthritis is an appropriate candidate. Clinicians must screen carefully before recommending this treatment. The following situations are contraindications or reasons for caution:
Active infection in or near the knee joint rules out the procedure entirely. Introducing a permanent hydrogel into an infected joint would be dangerous.
Patients with inflammatory arthritis — such as rheumatoid arthritis or psoriatic arthritis — are not the target population. Arthrosamid addresses the mechanical and synovial factors in osteoarthritis. Inflammatory joint disease involves different pathology.
Patients on anticoagulant therapy face a higher bleeding risk with any injection. Their medication and clotting status need careful review beforehand.
Patients with severe osteoarthritis and significant joint space loss are unlikely to achieve meaningful benefit. The hydrogel works best when there is sufficient joint architecture remaining.
Pregnancy and breastfeeding are periods where this treatment should not proceed, as safety data in these populations does not exist.
What Should Patients Monitor After the Injection?
Patients should expect mild discomfort and some swelling in the first one to two weeks. This is normal. Applying ice, resting the joint, and avoiding high-impact activity in the immediate post-injection period supports recovery.
Patients should contact their clinic promptly if they notice:
- Severe pain that worsens significantly after the initial expected flare has settled
- Marked swelling that increases rather than decreases over time
- Signs of infection — fever, a hot joint, chills, or feeling generally unwell
- Any symptom that feels abnormal or causes concern
Early identification of a complication leads to much better outcomes. No patient should hesitate to report symptoms that seem unusual.
The Importance of Clinician Expertise
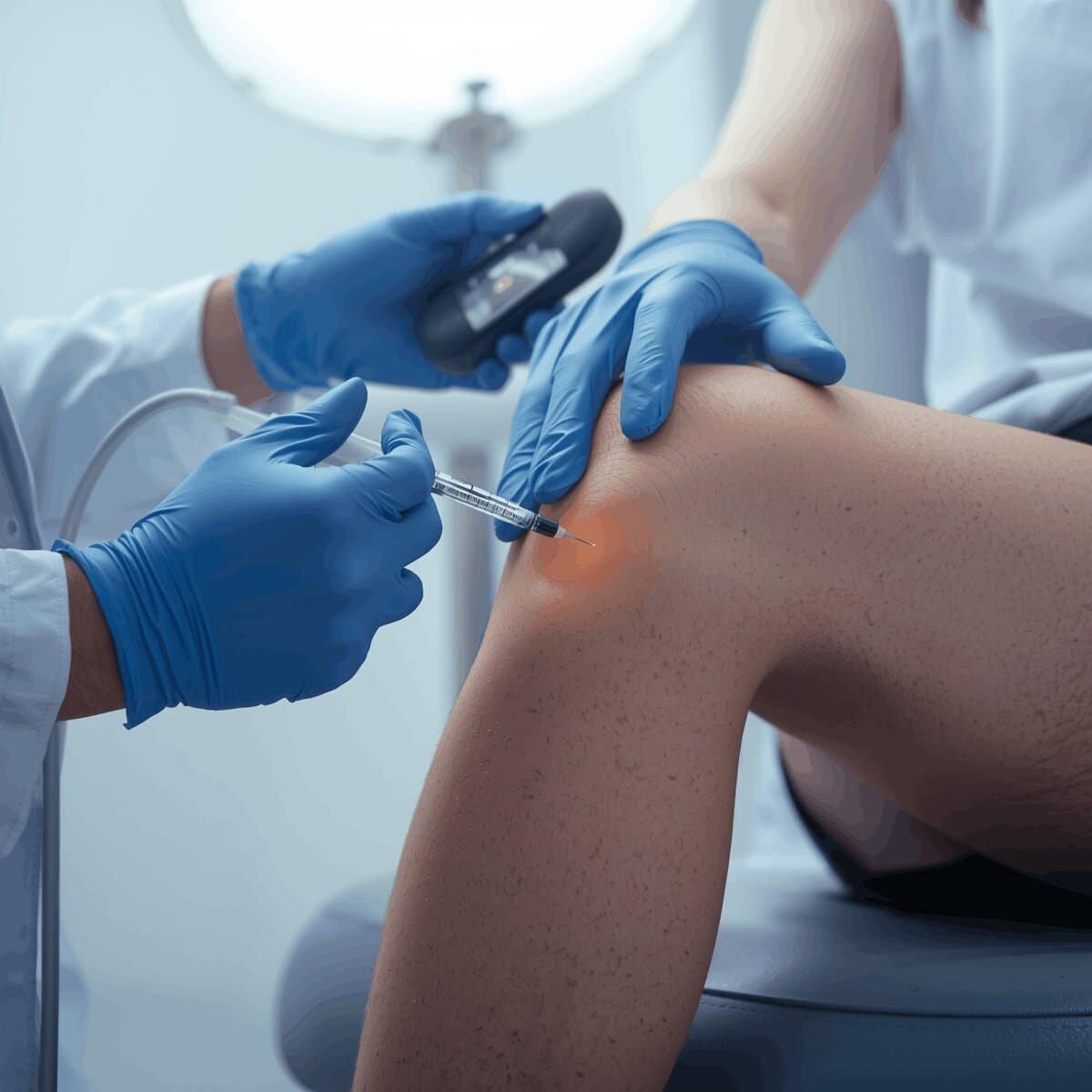
The safety and effectiveness of Arthrosamid depends not only on the product but on who delivers it. A healthcare provider must inject Arthrosamid under real-time ultrasound guidance to ensure accurate placement within the joint space. A poorly placed injection increases the risk of complications and reduces the chance of benefit.
Patients searching for Arthrosamid injection London or Arthrosamid injections near me should look beyond location and price. They should ask about the clinician’s training, their experience with intra-articular injections, and whether ultrasound guidance is used as standard.
At DRSNA Clinic on Harley Street, Dr Syed Nadeem Abbas — who holds an MSc in Aesthetic Plastic Surgery with Distinction from Queen Mary University London and trained at Cambridge, Oxford, and the Royal London Hospital — leads procedures to the standards expected at a Harley Street practice.
Arthrosamid Injection Cost in the UK: What Patients Should Know
Because Arthrosamid sits entirely outside NHS provision, every patient meets the full cost privately. Arthrosamid injection cost in the UK £2,800 per knee. Arthrosamid injection cost in London generally falls toward the upper end of this range, reflecting the overheads of central London clinical practice.
Some clinics bundle the initial consultation, the injection procedure, imaging, and post-procedure follow-up into a single package price. Others charge these elements separately. Patients researching arthrosamid injection cost UK should always request a complete breakdown before making any commitment.
Arthrosamid injection cost should not be the primary deciding factor. A lower price at a clinic that lacks adequate ultrasound equipment, sterile facilities, or a clinician with relevant training represents a false economy. The risks of the procedure increase significantly when corners are cut.
Patients using search terms such as arthrosamid injection near me or Arthrosamid Injection London will find a growing number of clinics offering this treatment. The growth in availability makes careful selection more important, not less.
An Honest Summary of the Risk Profile
Arthrosamid is not without risks. No injectable treatment is. The honest picture is this: for the majority of carefully selected patients, the side effects are mild, temporary, and manageable. Serious complications are uncommon when the procedure is performed correctly.
The permanent nature of the hydrogel is the single most important factor that distinguishes Arthrosamid from other intra-articular treatments. It is neither a reason to avoid the treatment nor a reason to be complacent. It is a reason to be fully informed before proceeding.
The evidence base, anchored by the TACIT trial, is credible and encouraging. It is also still growing. Patients who proceed do so at an earlier stage of the post-market evidence cycle than those who might consider this treatment in five- or ten-years’ time when longer-term data will be available.
That is neither a reason to refuse the treatment nor to rush into it. It is simply context that belongs in every informed consent discussion.
Arthrosamid offers a legitimate treatment option for adults with knee osteoarthritis who have not found adequate relief through conventional approaches. Its side effect profile, based on current evidence, is broadly acceptable. Mild reactions in the first two weeks are common and expected. Serious complications are rare but real, and patients must know the warning signs.
The most important determinants of a safe outcome are accurate patient selection, proper clinical technique, and a clinician with the right training and equipment. Arthrosamid injection cost in the UK places this treatment firmly in the private sector, which means patients carry the full responsibility of choosing the right clinic.
Read More:
Is Arthrosamid Injection the Right Knee Pain Treatment for You?
Arthrosamid Injection vs Steroid and Hyaluronic Acid Injections for Knee Pain